Abstract
Filed under: Cushing's, pituitary, Rare Diseases | Tagged: Acromegaly, cortisol, Cushing's Disease, dexamethasone suppression test, diabetes mellitus, growth hormone, hypertension, MRI, Pituitary adenoma | Leave a comment »
Filed under: Cushing's, pituitary, Rare Diseases | Tagged: Acromegaly, cortisol, Cushing's Disease, dexamethasone suppression test, diabetes mellitus, growth hormone, hypertension, MRI, Pituitary adenoma | Leave a comment »
Cushing’s syndrome, or endogenous hypercortisolemia, is a rare condition that both general practice clinicians and endocrinologists should be prepared to diagnose and treat. Including both the pituitary and adrenal forms of the disease, the Endocrine Society estimates that the disorder affects 10 to 15 people per million every year in the United States. It is more common in women and occurs most often in people between the ages of 20 and 50.
Even though Cushing’s remains a rare disease, cortisol recently made waves at the American Diabetes Association 84th Scientific Session. A highlight of the meeting was the initial presentation of data from the CATALYST trial, which assessed the prevalence of hypercortisolism in patients with difficult-to-control type 2 diabetes (A1c 7.5+).
CATALYST is a prospective, Phase 4 study with two parts. In the prevalence phase, 24% of 1,055 enrolled patients had hypercortisolism, defined as an overnight dexamethasone suppression test (ODST) value greater than 1.8 µg/dL and dexamethasone levels greater than 140 µg/dL. Results of CATALYST’s randomized treatment phase are expected in late 2024.
Elena Christofides, MD, FACE, founder of Endocrinology Associates, Inc., in Columbus, OH, believes the CATALYST results will be a wake-up call for both physicians and patients seeking to advocate for their own health. “This means that nearly 1 in 4 patients with type 2 diabetes have some other underlying hormonal/endocrine dysfunction as the reason for their diabetes, or significant contribution to their diabetes, and they should all be screened,” she said. “All providers need to get comfortable with diagnosing and treating hypercortisolemia, and you need to do it quickly because patients are going to pay attention as well.”
In Dr. Christofides’ experience, patients who suspect they have a hormonal issue may start with their primary care provider or they may self-refer to an endocrinologist. “A lot of Cushing’s patients are getting diagnosed and treated in primary care, which is completely appropriate. But I’ve also met endocrinologists who are uncomfortable diagnosing and managing Cushing’s because it is so rare,” she said. “The important thing is that the physician is comfortable with Cushing’s or is willing to put in the work get comfortable with it.”
According to Dr. Christofides, the widespread popular belief that “adrenal fatigue” is causing millions of Americans to feel sick, tired, and debilitated may be creating barriers to care for people who may actually have Cushing’s. “As physicians, we know that adrenal fatigue doesn’t exist, but we should still be receptive to seeing patients who raise that as a concern,” said Dr. Christofides. “We need to acknowledsalige their lived experience as being very real and it can be any number of diseases causing very real symptoms. If we don’t see these patients, real cases of hypercortisolemia could be left undiagnosed and untreated.”
Dr. Christofides, who also serves as a MedCentral Editor-at-Large, said she reminds colleagues that overnight dexamethasone suppression test (ODST) should always be the first test when you suspect Cushing’s. “While technically a screening test, the ODST can almost be considered diagnostic, depending on how abnormal the result is,” she noted. “But I always recommend that you do the ODST, the ACTH, a.m. cortisol, and the DHEAS levels at the same time because it allows you to differentiate more quickly between pituitary and adrenal problems.”
Dr. Christofides does see a place for 24-hour urine collection and salivary cortisol testing at times when diagnosing and monitoring patients with Cushing’s. “The 24-hour urine is only positive in ACTH-driven Cushing’s, so an abnormal result can help you identify the source, but too many physicians erroneously believe you can’t have Cushing’s if the 24-hour urine is normal,” she explained. “Surgeons tend to want this test before they operate and it’s a good benchmark for resolution of pituitary disease.” She reserves salivary cortisol testing for cases when the patient’s ODST is negative, but she suspects Cushing’s may be either nascent or cyclical.
Surgical resection has long been considered first-line treatment in both the pituitary and adrenal forms of Cushing’s. For example, data shared from Massachusetts General Hospital showed that nearly 90% of patients with microadenomas did not relapse within a 30-year period. A recent study found an overall recurrence rate of about 25% within a 10-year period. When reoperation is necessary, remission is achieved in up to 80% of patients.
As new medications for Cushing’s syndrome have become available, Dr. Christofides said she favors medical intervention prior to surgery. “The best part about medical therapy is you can easily stop it if you’re wrong,” she noted. “I would argue that every patient with confirmed Cushing’s deserves nonsurgical medical management prior to a consideration of surgery to improve their comorbidities and surgical risk management, and give time to have a proper informed consent discussion.”
In general, medications to treat Cushing’s disease rely on either cortisol production blockade or receptor blockade, said Dr. Christofides. Medications that directly limit cortisol production include ketoconazole, osilodrostat (Isturisa), mitotane (Lysodren), levoketoconazole (Recorlev), and metyrapone (Metopirone). Mifepristone (Korlym, Mifeprex) is approved for people with Cushing’s who also have type 2 diabetes to block the effects of cortisol. Mifepristone does not lower the amount of cortisol the body makes but limits its effects. Pasireotide (Signifor) lowers the amount of ACTH from the tumor. Cabergoline is sometimes used off-label in the US for the same purpose.
Following surgery, people with Cushing’s need replacement steroids until their adrenal function resumes, when replacement steroids must be tapered. But Dr. Christofides said she believes that all physicians who prescribe steroids should have a clear understanding of when and how to taper patients off steroids.
“Steroid dosing for therapeutic purposes is cumulative in terms of body exposure and the risk of needing to taper. A single 2-week dose of steroids in a year does not require a taper,” she said. “It’s patients who are getting repeated doses of more than 10 mg of prednisone equivalent per day for 2 or more weeks multiple times per year who are at risk of adrenal failure without tapering.”
Physicians often underestimate how long a safe, comfortable taper can take, per Dr. Christofides. “It takes 6 to 9 months for the adrenals to wake up so if you’re using high-dose steroids more frequently, that will cause the patient to need more steroids more frequently,” she explained. “If you’re treating an illness that responds to steroids and you stop them without tapering, the patient’s disease will flare, and then a month from then to 6 weeks from then you’ll be giving them steroids again, engendering a dependence on steroids by doing so.”
When developing a steroid taper plan for postoperative individuals with Cushing’s (and others), Dr. Christofides suggests basing it on the fact that 5 mg of prednisone or its equivalent is the physiologic dose. “Reduce the dose by 5 mg per month until you get to the last 5 mg, and then you’re going to reduce it by 1 mg monthly until done,” she said. “If a patient has difficulty during that last phase, consider a switch to hydrocortisone because a 1 mg reduction of hydrocortisone at a time may be easier to tolerate.”
Prednisone, hydrocortisone, and the other steroids have different half-lives, so you’ll need to plan accordingly, adds Dr. Christofides. “If you do a slower taper using hydrocortisone, the patient might feel worse than with prednisone unless you prescribe it BID.” She suggests thinking of the daily prednisone equivalent of hydrocortisone as 30 mg to allow for divided dosing, rather than the straight 20 mg/day conversion often used.
What happens after a patient’s Cushing’s has been successfully treated? Cushing’s is a chronic disease, even in remission, Dr. Christofides emphasized. “Once you have achieved remission, my general follow-up is to schedule visits every 6 months to a year with scans and labs, always with the instruction if the patient feels symptomatic, they should come in sooner,” she said.
More on Cushing’s diagnosis and therapies.
https://www.medcentral.com/endocrinology/cushings-syndrome-a-clinical-update
Filed under: adrenal, adrenal crisis, Cushing's, Diagnostic Testing, pituitary, Treatments | Tagged: 24-hour urine free cortisol test, ACTH, Adrenal fatigue, cabergoline, CATALYST trial, Cushing's Syndrome, cyclical, dexamethasone suppression test, DHEAS, diabetes, Dr. Elena Christofides, endocrinologist, Endocrinology Associates, hypercortisolism, Isturisa, ketoconazole, Korlym, levoketoconazole, Lysodren, Metopirone, Metyrapone, Mifeprex, mifepristone, mitotane, ODST, Osilodrostat, pasireotide, RECORLEV, salivary test, Signifor, steroids, surgery, taper, UFC, wean | Leave a comment »
Cushing’s syndrome is associated with excessive cortisol production and, if left untreated, can result in severe complications, such as heart attacks, strokes, and type 2 diabetes. To diagnose this condition, a dexamethasone suppression test is commonly performed.
Various factors, such as metabolic rate and interactions with other medications, can affect test efficacy. Therefore, it is crucial to measure the concentration of dexamethasone concurrently with cortisol to avoid false-positive results.
To address this issue, a team of researchers at the University of Turin, led by Professor Giulio Mengozzi in the Department of Medical Sciences, has developed a liquid chromatography-tandem mass spectrometry method.
This new method enables the simultaneous quantification of cortisol, cortisone, dexamethasone, and six additional exogenous corticosteroids, leading to a more accurate diagnosis of Cushing’s syndrome.
Cushing’s syndrome is a medical condition characterized by an abnormal and prolonged increase in cortisol production, typically affecting females between the ages of 30 and 50.1
While the issue may originate from within the body (endogenous), it is more commonly caused by external factors, such as the use of glucocorticoid medications.
Visible symptoms of Cushing’s syndrome include weight gain, an accumulation of fat around the base of the neck, a fatty hump between the shoulders, the appearance of a “moon face”, and easy bruising. However, not all individuals with the syndrome exhibit these symptoms, rendering diagnosis challenging. Without timely treatment, Cushing’s syndrome can lead to severe complications, including heart attack, stroke, blood clots in the legs and lungs, increased susceptibility to infections, memory loss, and type 2 diabetes.
A commonly used method for diagnosing Cushing’s syndrome is the dexamethasone suppression test (DST), which measures the adrenal gland’s response to adrenocorticotropic hormone (ACTH).
ACTH regulates cortisol levels in the blood plasma and stimulates the adrenal cortex to produce cortisol. When cortisol levels increase, ACTH secretion is suppressed. Dexamethasone, a synthetic steroid similar to cortisol, is administered during the DST to lower ACTH levels.
DSTs are available in low-dose (LDDST) and high-dose (HDDST). They can be performed overnight or over two days.
LDDSTs are used initially to diagnose Cushing’s syndrome. If the result is positive, HDDSTs help classify the disease as ACTH-dependent or independent. These tests are typically conducted in the following manner.2
Cortisol is a steroid hormone of the glucocorticoid class made by the adrenal glands.
Image Credit: Shutterstock/Kateryna Kon
Patients whose pituitary glands produce excessive amounts of ACTH will exhibit an abnormal response to the low-dose test but a normal reaction to the high-dose test.
During the LDDST, cortisol levels should decrease following the administration of dexamethasone, and a cut-off value of below 18 ng/mL is recommended to distinguish a healthy response from an unhealthy one.
For the HDDST, a decrease in urine-free cortisol (UFC) or serum cortisol greater than 50% indicates the presence of ACTH-dependent Cushing’s syndrome. This rule applies to both the overnight LDDST and the two-day HDDST methods.
Chemiluminescence immunoassay (CLIA) is a widely used method for measuring cortisol and other steroids due to its simplicity, automation, and good sensitivity.
However, it has some drawbacks, including cross-reactivity leading to overestimation of target analyte levels, non-standardization of kits, and the inability to measure more than one analyte per analysis. This is particularly problematic since studies indicate that measuring dexamethasone in combination with cortisol can reduce the number of false-positive DST results and improve interpretability. 3,4,5
Liquid chromatography-tandem mass spectrometry (LC-MS/MS) has emerged as a popular alternative to CLIA for DSTs due to its ability to measure multiple analytes simultaneously and its superior specificity.
Analytes are separated via LC, and their concentrations are measured by MS, with triple quadrupole MS configurations commonly used for this purpose. This technique provides the ability to measure multiple analytes simultaneously, along with higher accuracy and sensitivity than CLIA.
In the Division of Endocrinology, Diabetes, and Metabolism at the University of Turin, a team has developed an LC-MS/MS technique for simultaneous quantifying cortisol, cortisone, dexamethasone, and six other exogenous corticosteroids in serum/plasma samples.6
This method can be readily applied in any clinical laboratory equipped with a mass spectrometer and is effective in DSTs, enabling precise measurements of the target analytes in a single chromatographic run (Figure 1).
The study demonstrated a strong correlation between the results obtained from the newly developed LC-MS/MS method and those obtained using a commercially available CE IVD-marked Steroid Panel LC-MS* kit (Tecan).
The Tecan kit enables simultaneous dexamethasone, cortisol, and cortisone measurement and includes all the necessary components for easy implementation, such as calibrators and controls. The samples are prepared using solid-phase extraction (SPE), which can be semi-automatically performed on a Resolvex® A200 positive pressure processor (Tecan). The kit can measure 15 other steroids in the core steroid metabolism pathway due to the effectiveness of the SPE process.
Table 1. LC gradient elution programme. Source: Tecan
| Time (min) | Mobile phase A (%) | Mobile phase B (%) |
|---|---|---|
| 0 | 90 | 10 |
| 0.5 | 65 | 35 |
| 4.5 | 65 | 35 |
| 4.51 | 35 | 65 |
| 6.0 | 2 | 98 |
| 8.0 | 2 | 98 |
| 8.01 | 90 | 10 |
| 10.0 | 90 | 10 |
* In USA: for research use only. Not for use in diagnostic procedures. Product availability and regulatory status may vary from country to country. Consult with your Tecan associate for further information.
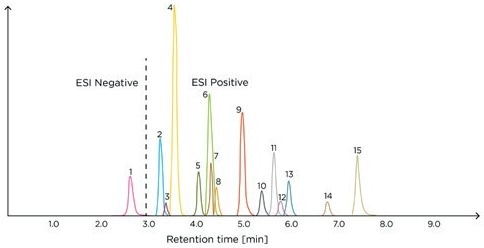
Figure 1. Example chromatogram of the Steroid Panel LC-MS internal standard – run 1. ESI, electrospray ionization; 1, aldosterone; 2, cortisone; 3, dehydro-epiandrosterone sulfate; 4, cortisol; 5, 21-deoxycortisol; 6, corticosterone; 7, dexamethasone; 8, 11-deoxycortisol; 9, androstenedione; 10, 11-deoxycorticosterone; 11, testosterone; 12, dehydroepiandrosterone; 13, 17-hydroxyprogesterone; 14, dihydrotestosterone; 15, progesterone.
Image Credit: Tecan
Early diagnosis of Cushing’s syndrome is critical to prevent potentially fatal complications. A reliable method for reducing the number of false positives in DSTs involves the simultaneous measurement of cortisol and dexamethasone levels, which can be accurately achieved using LC-MS/MS.
The LC-MS/MS method described in this article enables the simultaneous measurement of multiple analytes, such as cortisol, cortisone, and dexamethasone, in serum or plasma.
This analytical approach can provide clinical laboratories with a straightforward method for performing DSTs, and the commercially available kit can ensure consistent and dependable results.
Filed under: Cushing's, Diagnostic Testing, symptoms | Tagged: cortisol, dexamethasone suppression test, diabetes, heart attack, stroke | Leave a comment »
Even in the face of overt clinical signs and symptoms of hypercortisolism, diagnosing Cushing syndrome requires a high index of suspicion, and people with hypercortisolism experience a long road to diagnosis. In a recent meta-analysis including more than 5000 patients with Cushing syndrome, the mean time to diagnosis in all Cushing syndrome, including Cushing disease and ectopic adrenocorticotropin (ACTH) syndrome, was 34 months (1). Reasons for delayed diagnosis are multifactorial, including the nonspecific nature of subjective symptoms and objective clinical signs, as well as notorious challenges in the interpretation of diagnostic testing. Furthermore, the health care system’s increasingly organ-specific referral patterns obfuscate multisystem disorders. Improving the recognition of and decreasing time to diagnosis in Cushing syndrome are critical factors in reducing morbidity and mortality.
Here, we present the case of a patient who, despite classic signs of Cushing syndrome as well as progressive physical and mental decline, remained undiagnosed for more than 3 years while undergoing repeated evaluation by primary care and subspecialty providers. The case (1) highlights the lack of awareness of Cushing syndrome as a potential unifying diagnosis for multiorgan system problems; (2) underscores the necessity of continued education on the signs and symptoms of hypercortisolism, appropriate screening for hypercortisolism, and early referral to endocrinology; and (3) provides an opportunity for systemic change in clinical laboratory practice that could help improve recognition of pathologic hypercortisolism.
In August 2018, a previously healthy 40-year-old man with ongoing tobacco use established care with a primary care provider complaining that he had been ill since the birth of his son 13 months prior. He described insomnia, headaches, submandibular swelling, soreness in his axillary and inguinal regions, and right-sided chest discomfort (Fig. 1). Previously, he had been diagnosed with sinusitis, tonsillitis, and allergies, which had been treated with a combination of antibiotics, antihistamines, and intranasal glucocorticoids. He was referred to otolaryngology where, in the absence of cervical lymphadenopathy, he was diagnosed with sternocleidomastoid pain with recommendations to manage conservatively with stretching and massage. A chest x-ray demonstrated a left apical lung nodule. Symptoms continued unabated throughout 2019, now with a cough. Repeat chest x-ray demonstrated opacities lateral to the left hilum that were attributed to vascular structures.
Timeline of development of subjective symptoms and objective clinical findings preceding diagnosis and surgical cure of ectopic Cushing syndrome.
In May 2020, increasingly frustrated with escalating symptoms, the patient transitioned care to a second primary care provider and was diagnosed with hypertension. He complained of chronic daily headaches that prompted brain imaging with magnetic resonance imaging (MRI), which noted findings consistent with left maxillary silent sinus syndrome. He was sent back to otolaryngology, which elected to proceed with sinus surgery. During this time, he suffered a fibular fracture for which he was evaluated by orthopedic surgery. In the second half of 2020, he was seen by neurology to evaluate his chronic headaches and paresthesias with electromyography demonstrating a left ulnar mononeuropathy consistent with cubital tunnel syndrome. His primary care provider diagnosed him with fibromyalgia for which he started physical therapy, and he was referred to a pain clinic for cognitive behavioral therapy. Unfortunately his wife, dealing with her husband’s increasing cognitive and personality changes including irritability and aggression, filed for divorce.
At the end of 2020, the patient developed bilateral lower extremity edema and was prescribed hydrochlorothiazide, subsequently developing hypokalemia attributed to diuretic use. With worsening bilateral lower extremity edema and new dyspnea on exertion, he was evaluated for heart failure with an echocardiogram, which was unremarkable. Over the next several months, he gained approximately 35 pounds (∼16 kg). It was in the setting of weight gain that he was first evaluated for hypercortisolism with random serum cortisol of 22.8 mcg/dL (629 nmol/L) and 45.6 mcg/dL (1258 nmol/L) in the late morning and mid-day, respectively. No reference range was provided for the times of day at which these laboratory values were drawn. Although these serum cortisol values were above provided reference ranges for other times of day, they were not flagged as abnormal by in-house laboratory convention, and they were overlooked. The search for other etiologies of his symptoms continued.
In early 2021, diuretic therapy and potassium supplementation were escalated for anasarca. He developed lower extremity cellulitis and received multiple courses of antibiotics. Skin biopsy performed by dermatology demonstrated disseminated Mycobacterium and later Serratia (2), prompting referral to infectious disease for management. Additional subspecialty referrals included rheumatology (polyarthralgia) and gastroenterology (mildly elevated alanine transaminase with planned liver biopsy). In July 2021, he was evaluated for edema by nephrology, where the constellation of subjective symptoms and objective data including hypertension, central weight gain, abdominal striae, fracture, edema, easy bruising, medication-induced hypokalemia, atypical infections, and high afternoon serum cortisol were noted, and the diagnosis of Cushing syndrome was strongly suspected. Emergent referral to endocrinology was placed.
At his first clinic visit with endocrinology in June 2021, the patient’s blood pressure was well-controlled on benazepril. Following weight gain of 61 pounds (∼28 kg) in the preceding 2 years, body mass index was 33. Physical examination demonstrated an ill-appearing gentleman with dramatic changes when compared to prior pictures (Fig. 2), including moon facies, dorsocervical fat pad, violaceous abdominal striae, weeping lower extremity skin infections, an inability to stand without assistance from upper extremities, and depressed mood with tangential thought processes.
Photographic representation of physical changes during the years leading up to diagnosis of ectopic Cushing syndrome in June 2021 and after surgical resection of culprit lesion.
Diagnostic workup for hypercortisolism included a morning cortisol of 33.4 mcg/dL (922 nmol/L) (normal reference range, 4.5-22.7 mcg/dL) and ACTH of 156 pg/mL (34 pmol/L) (normal reference range, 7.2-63 pg/mL) following bedtime administration of 1-mg dexamethasone, and 24-hour urine free cortisol of 267 mcg/24 hours (737 nmol/24 hours) (normal reference range, 3.5-45 mcg/24 hours). Morning serum cortisol and plasma ACTH following bedtime administration of 8-mg dexamethasone were 27.9 mcg/dL (770 nmol/L) and 98 pg/mL (22 pmol/L), respectively. Given concern for potential decompensation, he was hospitalized for expedited work-up. Brain MRI did not demonstrate a pituitary lesion (Fig. 3), and inferior petrosal sinus sampling under desmopressin stimulation showed no central-to-peripheral gradient (Table 1). He underwent a positron emission tomography–computed tomography 68Ga-DOTATATE scan that demonstrated a 1.2-cm left pulmonary nodule with radiotracer uptake (Fig. 4).
A, Precontrast and B, postcontrast T1-weighted sagittal magnetic resonance imaging of the sella. Images were affected by significant motion degradation, precluding clear visualization of the pituitary gland on coronal imaging.
68Ga-DOTATATE imaging. A, Coronal and B, axial views of the chest after administration of radiopharmaceutical. Arrow in both panels indicates DOTATATE-avid 1.2-cm left lung lesion.
Bilateral petrosal sinus and peripheral adrenocorticotropin levels preintravenous and postintravenous injection of desmopressin acetate 10 mcg
| Time post DDAVP, min | Left petrosal ACTH | Left petrosal:peripheral ACTH | Right petrosal ACTH | Right petrosal:peripheral ACTH | Peripheral ACTH | Left:right petrosal ACTH |
|---|---|---|---|---|---|---|
| 0 | 172 pg/mL (37.9 pmol/L) |
1.1 | 173 pg/mL (38.1 pmol/L) |
1.2 | 150 pg/mL (33.0 pmol/L) |
1.0 |
| 3 | 288 pg/mL (63.4 pmol/L) |
1.8 | 292 pg/mL (64.3 pmol/L) |
1.8 | 162 pg/mL (35.7 pmol/L) |
1.0 |
| 5 | 348 pg/mL (76.6 pmol/L) |
1.8 | 341 pg/mL (75.1 pmol/L) |
1.8 | 191 pg/mL (42.1 pmol/L) |
1.0 |
| 10 | 367 pg/mL (80.8 pmol/L) |
1.3 | 375 pg/mL (82.6 pmol/L) |
1.3 | 278 pg/mL (61.2 pmol/L) |
1.0 |
Abbreviations: ACTH, adrenocorticotropin; DDAVP, desmopressin acetate.
The patient was started on ketoconazole 200 mg daily for medical management of ectopic ACTH-induced hypercortisolism while awaiting definitive surgical treatment. Within a month of initial endocrinology evaluation, he underwent thoracoscopic left upper lobe wedge resection with intraoperative frozen histopathology section consistent with a well-differentiated neuroendocrine tumor and final pathology consistent with a well-differentiated neuroendocrine tumor. Staining for ACTH was positive (Fig. 5). Postoperative day 1 morning cortisol was 1.4 mcg/dL (39 nmol/L) (normal reference range, 4.5-22.7 mcg/dL). He was started on glucocorticoid replacement with hydrocortisone and was discharged from his surgical admission on hydrocortisone 40 mg in the morning and 20 mg in the afternoon.
Lung tumor histopathology. A, The tumor was epicentered around a large airway (asterisk) and showed usual architecture for carcinoid tumor. B, The tumor cells had monomorphic nuclei with a neuroendocrine chromatin pattern, variably granulated cytoplasm, and a delicate background vascular network. By immunohistochemistry, the tumor cells were strongly positive for C, synaptophysin; D, CAM5.2; and E, adrenocorticotropin. F, Ki-67 proliferative index was extremely low (<1%).
Approximately 12 days after discharge, the patient was briefly readmitted from the skilled nursing facility where he was receiving rehabilitation due to a syncopal event attributed to hypovolemia. This was felt to be secondary to poor oral intake in the setting of both antihypertensive and diuretic medications as well as an episode of emesis earlier in the morning precluding absorption of his morning hydrocortisone dose. Shortly after this overnight admission, he was discharged from his skilled nursing facility to home. In the first month after surgery, he lost approximately 30 pounds (∼14 kg) and had improvements in sleep and mood.
Eight months after surgery, hydrocortisone was weaned to 10 mg daily. Cosyntropin stimulation testing holding the morning dose showed 1 hour cortisol 21.5 mcg/dL (593 nmol/L). Hydrocortisone was subsequently discontinued. In June 2022, 1 year following surgery, 3 sequential midnight salivary cortisol tests were undetectable. At his last visit with endocrinology in June 2023, he felt well apart from ongoing neuropathic pain in his feet and continued but improved mood disturbance. Though his health has improved dramatically, he continues to attribute his divorce and substantial life disruption to his undiagnosed hypercortisolism.
Endogenous neoplastic hypercortisolism encompasses a clinical spectrum from subclinical disease, as is common in benign adrenal cortical adenomas, to overt Cushing syndrome of adrenal, pituitary, and ectopic origin presenting with dramatic clinical manifestations (3) and long-term implications for morbidity and mortality (4). Even in severe cases, a substantial delay in diagnosis is common. In this case, despite marked hypercortisolism secondary to ectopic ACTH syndrome, the patient’s time from first symptoms to diagnosis was more than 3 years, far in excess of the typical time to diagnosis in this subtype, noted to be 14 months in 1 study (1).
He initially described a constellation of somatic symptoms including subjective neck swelling, axillary and inguinal soreness, chest discomfort, and paresthesias, and during the year preceding diagnosis, he developed hypertension, fibular fracture, mood changes, weight gain, peripheral edema, hypokalemia, unusual infections, and abdominal striae. Each of these symptoms in isolation is a common presentation in the primary care setting, therefore the challenge arises in distinguishing common, singular causes from rare, unifying etiologies, especially given the present epidemics of diabetes, obesity, and associated cardiometabolic abnormalities. By Endocrine Society guidelines, the best discriminatory features of Cushing syndrome in the adult population are facial plethora, proximal muscle weakness, abdominal striae, and easy bruising (5). Furthermore, Endocrine Society guidelines suggest evaluating for Cushing disease when consistent clinical features are present at a younger-than-expected age or when these features accumulate and progress, as was the case with our patient (5).
However, even when the diagnosis is considered, the complexities of the hypothalamic-pituitary-adrenal axis make selection and interpretation of screening tests challenging outside the endocrinology clinic. We suspect that in most such situations, a random serum cortisol measurement is far more likely to be ordered than a validated screening test, such as dexamethasone suppression testing, urine free cortisol, and late-night salivary cortisol per Endocrine Society guidelines (5). Although random serum cortisol values are not considered a screening test for Cushing syndrome, elevated values can provide a clue to the diagnosis in the right clinical setting. In this case, 2 mid-day serum cortisols were, by in-house laboratory convention, not flagged as abnormal despite the fact that they were above the upper limit of provided reference ranges. We suspect that the lack of electronic medical record flagging of serum cortisol values contributed to these values being incorrectly interpreted as ruling out the diagnosis.
Cushing syndrome remains among the most evasive and difficult diagnoses in medicine due to the doubly difficult task of considering the disorder in the face of often protean signs and symptoms and subsequently conducting and interpreting screening tests. The challenges this presents for the nonendocrinologist have recently been recognized by a group in the United Kingdom after a similarly overlooked case (6). We believe that our case serves as a vivid illustration of the diagnostic hurdles the clinician faces and as a cautionary tale with regard to the potential downstream effects of a delay in diagnosis. Standardization of clinical laboratory practices in flagging abnormal cortisol values is one such intervention that may aid the busy clinician in more efficiently recognizing laboratory results suggestive of this diagnosis. While false-positive case detection is a significant downside to this approach, given the potential harm in delayed or missed diagnosis, the potential benefits may outweigh the risks.
We are grateful to the patient for allowing us to present his difficult case to the community with the hopes of improving time to diagnosis for patients with hypercortisolism.
All authors made individual contributions to authorship. J.M.E., E.M.Z., and K.R.K. were involved in the diagnosis and management of this patient. B.C.M., J.M.E., E.M.Z., and K.R.K. were involved in manuscript submission. S.M.J. performed and analyzed histopathology and prepared the figure for submission. All authors reviewed and approved the final draft.
No public or commercial funding.
J.M.E. was on the editorial board of JCEM Case Reports at the time of initial submission.
Signed informed consent obtained directly from the patient.
Data sharing is not applicable to this article as no data sets were generated or analyzed during the current study.
,
,
, et al.
.
.
;
(
):
.
,
,
,
,
.
.
.
;
:
‐
.
,
.
.
.
;
(
):
‐
.
,
,
, et al.
.
.
;
(
):
‐
.
,
,
,
,
,
.
.
.
;
(
):
‐
.
adrenocorticotropin
magnetic resonance imaging
Filed under: Cushing's, Diagnostic Testing, Rare Diseases | Tagged: 68Ga-DOTATATE scan, dexamethasone suppression test, ectopic, Ectopic Cushing’s syndrome, lung | Leave a comment »
The aim of this study was to investigate the clinical features and treatment options for pediatric adrenal incidentalomas(AIs) to guide the diagnosis and treatment of these tumors.
The clinical data of AI patients admitted to our hospital between December 2016 and December 2022 were collected and retrospectively analyzed. All patients were divided into neonatal and nonneonatal groups according to their age at the time of the initial consultation.
In the neonatal group, 13 patients were observed and followed up, and the masses completely disappeared in 8 patients and were significantly reduced in size in 5 patients compared with the previous findings. Four patients ultimately underwent surgery, and the postoperative pathological diagnosis was neuroblastoma in three patients and teratoma in one patient. In the nonneonatal group, there were 18 cases of benign tumors, including 9 cases of ganglioneuroma, 2 cases of adrenocortical adenoma, 2 cases of adrenal cyst, 2 cases of teratoma, 1 case of pheochromocytoma, 1 case of nerve sheath tumor, and 1 case of adrenal hemorrhage; and 20 cases of malignant tumors, including 10 cases of neuroblastoma, 9 cases of ganglioneuroblastoma, and 1 case of adrenocortical carcinoma.
Neuroblastoma is the most common type of nonneonatal AI, and detailed laboratory investigations and imaging studies are recommended for aggressive evaluation and treatment in this population. The rate of spontaneous regression of AI is high in neonates, and close observation is feasible if the tumor is small, confined to the adrenal gland and has no distant metastasis.
The incidence of adrenal incidentaloma (AI) is increasing due to the increased frequency of imaging and improved imaging sensitivity [1]. AI is relatively common in adults, and several organizations, such as the American Association of Clinical Endocrinologists/American Association of Endocrine Surgeons and the European Society Endocrinology, have proposed specific protocols to guide the evaluation, treatment, and follow-up management of AI in adults [2]. Although AI, a nonfunctioning adrenocortical adenoma, is most common in adults, neuroblastoma is the most common incidental tumor of the adrenal gland in children. In addition, in the neonatal period, which is a more complex stage of childhood, the biology of adrenal masses found in this age group is also more specific, and the nature of these masses can range from spontaneous regression to rapid progression to aggressive disease with metastatic dissemination and even death. Given that AI is the most common malignant tumor, the management of AI in children cannot be simply based on the measurements used in adult AI. In this study, we retrospectively analyzed the clinical data of pediatric AI patients in a single center to investigate the clinical characteristics and management of AI in children.
A total of 66 children with adrenal tumors were diagnosed and treated at the Department of Urology of the Children’s Hospital of Nanjing Medical University from December 2016 to December 2022. A total of 55 cases were detected during physical examination, or the patients were diagnosed and received treatment for diseases other than adrenal disease after excluding adrenal tumors detected due to typical clinical manifestations or signs such as centripetal obesity and precocious puberty. Research protocols involving human materials were approved by the Medical Ethics Committee of the Children’s Hospital of Nanjing Medical University. All clinical information, radiological diagnosis, laboratory test results, intervention results, and follow-up data were collected from the department’s database.
All the children underwent ultrasonography and CT scanning, and 11 children underwent MRI. In addition to routine tests such as blood routine and biochemical indexes, the examination and evaluation of adrenal endocrine hormones and tumor markers included (1) plasma cortisol and ACTH levels, (2) plasma catecholamine and metabolite determination, (3) plasma renin and plasma aldosterone, (4) urinary vanillylmandelic acid/homovanillic acid(VMA/HVA), and (5) AFP, CEA, NSE, and CA19-9. Five patients underwent a low-dose dexamethasone suppression test. Seventeen of the 55 patients were treated with watch-waiting therapy, 4 of the 17 ultimately underwent surgery, 4 of the 38 patients underwent tumor biopsy, and 34 underwent adrenalectomy.
The data were analyzed using Graph Pad Prism 8. The measurement data are expressed as ‾x ± sd. The maximum diameter of the tumors, age of the patients with benign and malignant tumors, and maximum diameter of the tumors between the laparoscopic surgery group and the open surgery group were compared using paired t tests, and the percentages of the count data were compared using Fisher’s exact test.
In this study, all patients were divided into two groups according to their age at the time of consultation: the neonate group and the nonneonate group.
Neonate group:
There were 7 male and 10 female patients, 7 of whom were diagnosed via prenatal examination and 10 of whom were diagnosed after birth. Five patients were diagnosed with lesions on the left side, 12 patients were diagnosed with lesions on the right side, and the maximal diameters of the masses ranged from 16 to 48 mm. The characteristics of the AIs in the neonate group are presented in Table 1.
Among the 17 patients, 8 had cystic masses with a maximum diameter of 16∼48 mm, 5 had cystic-solid masses with a maximum diameter of 33∼39 mm, and 4 had solid masses with a maximum diameter of 18∼45 mm. Two patients with solid adrenal gland masses suggested by CT scan had obvious elevations in serum NSE and maximum diameters of 44 and 45 mm, respectively. These patients underwent adrenal tumor resection, and the pathology diagnosed that they had neuroblastomas(NB). In one patient, the right adrenal gland was 26 × 24 × 27 mm in size with slightly elevated echogenicity at 38 weeks after delivery, and the mass increased to a size of 40 × 39 × 29 mm according to the 1-month postnatal review. MRI suggested that the adrenal gland tumor was associated with liver metastasis, and the pathology of the tumor suggested that it was NB associated with liver metastasis after surgical resection (stage 4 S, FH). One child was found to have 25 × 24 × 14 mm cystic echoes in the left adrenal region during an obstetric examination, and ultrasound revealed 18 × 11 mm cystic solid echoes 5 days after birth. Ultrasound revealed 24 × 15 mm cystic solid echoes at 2 months. Serum NSE and urinary VMA were normal, and the tumor was excised due to the request of the parents. Pathology suggested a teratoma in the postoperative period. A total of 13 children did not receive surgical treatment or regular review via ultrasound, serum NSE or urine VMA. The follow-up time ranged from 1 to 31 months, with a mean of 9.04 ± 7.61 months. Eight patients had complete swelling, and 5 patients were significantly younger than the previous patients. Nonneonate group:
There were 24 male and 14 female patients in the nonneonate group; 24 patients had lesions on the left side, 14 patients had lesions on the right side, and the maximal diameters of the masses ranged from 17 to 131 mm. Most of these tumors were found during routine physical examinations or incidentally during examinations performed for various complaints, such as gastrointestinal symptoms, respiratory symptoms, or other related conditions. As shown in Table 2, abdominal pain was the most common risk factor (44.7%) for clinical onset, followed by routine physical examination and examination for respiratory symptoms.
Among the 38 patients, 10 had NBs with maximum diameters ranging from 20 to 131 mm, 9 had ganglion cell neuroblastomas with maximum diameters ranging from 33.6 to 92 mm, 9 had ganglion cell neuromas with maximum diameters ranging from 33 to 62 mm, 2 had adrenal adenomas with maximum diameters ranging from 17 to 70 mm, 1 had a cortical carcinoma with a maximum diameter of 72 mm, 2 had adrenal cysts with maximum diameters ranging from 26 to 29 mm, 2 had mature teratomas with maximum diameters of 34 and 40 mm, 1 had a pheochromocytoma with a diameter of 29 mm, 1 had a nerve sheath tumor with a diameter of 29 mm, and 1 patient with postoperative pathological confirmation of partial hemorrhagic necrosis of the adrenal gland had focal calcification with a maximum diameter of 25 mm (Table 3).
The mean age of children with malignant tumors was significantly lower than that of children with benign tumors (57.95 ± 37.20 months vs. 105.0 ± 23.85 months; t = 4.582, P < 0.0001). The maximum diameter of malignant tumors ranged from 20 to 131 mm, while that of benign tumors ranged from 17 to 72 mm, and the maximum diameter of malignant tumors was significantly greater than that of benign tumors (65.15 ± 27.61 mm v 37.59 ± 12.98 mm; t = 3.863, P = 0.0004). Four biopsies, 5 laparoscopic adrenal tumor resections and 11 open adrenal tumor resections were performed for malignant tumors, and 16 laparoscopic adrenal tumor resections and 2 open procedures were performed for benign tumors. The maximum diameter of the tumors ranged from 17 to 62 mm in 21 children who underwent laparoscopic surgery and from 34 to 99 mm in 13 children who underwent open resection; there was a statistically significant difference in the maximum diameter of the tumors between the laparoscopic surgery group and the open surgery group (35.63 ± 10.36 mm v 66.42 ± 20.60 mm; t = 5.798, P < 0.0001).
Of the 42 children with definitive pathologic diagnoses at surgery, 23 had malignant tumors, and 19 had benign tumors. There were 15 malignant tumors with calcification on imaging and 5 benign tumors. The percentage of malignant tumors with calcifications in was significantly greater than that of benign tumors (65.22% v 26.32%; P = 0.0157). In the present study, all the children underwent CT, and 31 patients had postoperative pathological confirmation of NB. A total of 26 patients were considered to have neurogenic tumors according to preoperative CT, for a diagnostic compliance rate of 83.97%. Three children were considered to have cortical adenomas by preoperative CT, and 1 was ultimately diagnosed by postoperative pathology, for a diagnostic compliance rate of 33.33%. For 4 patients with teratomas and adrenal cysts, the CT findings were consistent with the postoperative pathology. According to our research, NB 9-110HU, GNB 15-39HU, GB 19-38HU, ACA 8HU, adrenal cyst 8HU, and cellular achwannoma 17HU.
According to the clinical practice guidelines developed by the European Society of Endocrinology and European Network for the Study of Adrenal Tumors, AI is an adrenal mass incidentally detected on imaging not performed for a suspected adrenal disease [3]. The prevalence of AI is approximately 4%, and the incidence increases with age [4]. Most adult AIs are nonfunctioning benign adrenal adenomas (up to 75%), while others include functioning adrenal adenomas, pheochromocytomas, and adrenocortical carcinomas [5]. In contrast to the disease spectrum of adult AI cases, NB is the most common tumor type among children with AI, and benign cortical adenomas, which account for the vast majority of adult AI, accounting for less than 0.5% of cases in children [6]. According to several guidelines, urgent assessment of an AI is recommended in children because of a greater likelihood of malignancy [3, 7].
When an adult patient is initially diagnosed with AI, it should be clear whether the lesion is malignant and functional. In several studies, the use of noncontrast CT has been recommended as the initial imaging method for adrenal incidentaloma; a CT attenuation value ≤ 10 HU is used as the diagnostic criterion for benign adenomas; and these methods have a specificity of 71-79% and a sensitivity of 96-98% [8, 9]. A CT scan of tumors with diameters greater than 4 to 6 cm, irregular margins or heterogeneity, a CT attenuation value greater than 10 HU, or a relative contrast enhancement washout of less than 40% 10 or 15 min after administration of contrast media on enhanced CT is considered to indicate potential malignancy [7]. As the most common AI in children, NB often appears as a soft tissue mass with uneven density on CT, often accompanied by high-density calcified shadows, low-density cystic lesions or necrotic areas. CT scans can easily identify more typical NBs, and for those AIs that do not show typical calcified shadows on CT, it is sometimes difficult to differentiate neurogenic tumors from adenomas. In these patients, except for the 1 patient with adrenal cysts who had a CT value of 8 HU, very few of the remaining AI patients had a CT value less than 10 HU. Therefore, the CT value cannot be used simply as a criterion for determining the benign or malignant nature of AI, and additional imaging examinations, such as CT enhancement, MRI, and FDG-PET if necessary, should be performed immediately for AI in children.
Initial hormonal testing is also needed for functional assessment, and aldosterone secretion should also be assessed when the patient is hypertensive or hypokalemic [7]. Patients with AI who are not suitable for surgery should be observed during the follow-up period, and if abnormal adrenal secretion is detected or suggestive of malignancy during this period, prompt adrenal tumor resection is needed. For adult patients with AI, laparoscopic adrenal tumor resection is one of the most effective treatments that has comparative advantages in terms of hospitalization time and postoperative recovery speed; however, there is still some controversy over whether to perform laparoscopic surgery for some malignant tumors with large diameters, especially adrenocortical carcinomas, and some studies have shown that patients who undergo laparoscopic surgery are more prone to peritoneal seeding of tumors [10].
The maximum diameter of an adult AI is a predictor of malignancy, and a study by the National Italian Study Group on Adrenal Tumors, which included 887 AIs, showed that adrenocortical carcinoma was significantly correlated with the size of the mass, and the sensitivity of detecting adrenocortical carcinoma with a threshold of 4 cm was 93% [11]. According to the National Institutes of Health, patients with tumors larger than 6 cm should undergo surgical treatment, while patients with tumors smaller than 4 cm should closely monitored; for patients with tumors between 4 and 6 cm, the choice of whether to be monitored or surgically treated can be based on other indicators, such as imaging [12]. A diameter of 4 cm is not the initial threshold for determining the benign or malignant nature of a mass in children.
In a study of 26 children with AI, Masiakos et al. reported that 9 of 18 benign lesions had a maximal diameter less than 5 cm, 4 of 8 malignant lesions had a maximal diameters less than 5 cm, and 2 had a diameter less than 3 cm. The mean maximal diameter of benign lesions was 4.2 ± 1.7 cm, whereas the mean maximum diameter of malignant lesions was 5.1 ± 2.3 cm. There was no statistically significant difference between the two comparisons; therefore, this study concluded that children with AI diameters less than 5 cm cannot be treated expectantly [6]. Additionally, this study revealed that malignant lesions occurred significantly more frequently than benign lesions in younger children (mean age 1.7 ± 1.8 years v 7.8 ± 5.9 years; P = 0.02).
In the nonneonatal group of this study, 20 patients with malignant tumors had maximum diameters ranging from 20 to 131 mm, 10 had malignant tumors larger than 60 mm, and 3 had tumors smaller than 40 cm; 18 patients with benign tumors had maximum diameters ranging from 17 to 70 mm, 5 had diameters ranging from 40 to 60 mm, and 5 had diameters larger than 60 mm. Therefore, it is not recommended to use the size of the largest diameter of the tumor to decide whether to wait and observe or intervene surgically for children with AI. Instead, it is necessary to consider the age of the child; laboratory test results, such as whether the tumor indices are elevated or not; whether the tumor has an endocrine function; etc.; and imaging test results to make comprehensive judgments and decisions. Preoperative aggressive evaluation and prompt surgical treatment are recommended for nonneonatal pediatric AI patients.
Adrenal hematoma and NBs are the most common types of adrenal area masses in children, while pheochromocytoma, adrenal cyst, and teratoma are rarer masses [13]. In clinical practice, adrenal hematoma and NB are sometimes difficult to differentiate, especially when adrenal masses are found during the prenatal examination and neonatal period, and such children need to be managed with caution. The Children’s Oncology Group (COG ANBL00B1) implemented the watchful waiting treatment for children under 6 months of age with a solid adrenal mass < 3.1 cm in diameter (or a cystic mass < 5 cm) without evidence of distant metastasis, and if there is a > 50% increase in the adrenal mass volume, there is no return to the baseline VMA or HVA levels, or if there is a > 50% increase in the urinary VMA/HVA ratio or an inversion, surgical resection should be performed [14]. Eighty-three children in this study underwent expectant observation, 16 of whom ultimately underwent surgical resection (8 with INSS stage 1 NB, 1 with INSS stage 2B, 1 with INSS stage 4 S, 2 with low-grade adrenocortical neoplasm, 2 with adrenal hemorrhage, and 2 with extralobar pulmonary sequestration). Most of the children who were observed had a reduced adrenal mass volume. Of the 56 patients who completed the final 90 weeks of expectant observation, 27 (48%) had no residual mass, 13 (23%) had a residual mass volume of 0–1 ml, 8 (14%) had a mass volume of 1–2 ml, and 8 (14%) had a volume of > 2 ml; ultimately, 71% of the residual masses had a volume ≤ 1 ml and 86% had a residual volume ≤ 2 ml. In this study, a total of 16 patients were included in the watchful waiting treatment group; 3 patients underwent surgical treatment during the follow-up period, and 13 patients ultimately completed watchful waiting treatment. After 1–31 months of follow-up, 8 patients’ swelling completely disappeared, and 5 patients’ swelling significantly decreased. After strict screening for indications and thorough follow-up review, AIs in the neonatal period can be subjected to watchful waiting treatment, and satisfactory results can be achieved.
For benign adrenal tumors, laparoscopic surgery is superior to open surgery in terms of successful resection, whereas the feasibility of minimally invasive surgery for AI with preoperative suspicion of malignancy is controversial. The European Cooperative Study Group for Pediatric Rare Tumors recommends that minimally invasive surgery be considered only for early childhood tumors and should be limited to small, localized tumors; additionally, imaging should suggest no invasion of surrounding tissue structures or lymph nodes; and this strategy requires surgeons with extensive experience in oncologic and adrenal surgery [15]. NB is the most common pediatric AI, and open tumor resection remains the mainstay of treatment. For small, early tumors without evidence of invasion on preoperative examination, laparoscopic resection may be considered if the principles of oncologic surgery can be adhered to. If the patient responds to chemotherapy, the decision to perform laparoscopic tumor resection can also be re-evaluated after chemotherapy. According to the current study, the recurrence and mortality rates of laparoscopic surgery are comparable to those of open surgery [16, 17]. The relative contraindications for laparoscopic NB resection include a tumor diameter greater than 6 cm, venous dilatation, and the involvement of adjacent organs or blood vessels [18]. Patients who undergo open adrenalectomy have higher overall survival and recurrence-free survival rates than patients who undergo laparoscopic adrenalectomy [19]. Open adrenalectomy remains the gold standard for surgical resection of adrenocortical carcinoma, whereas laparoscopic adrenalectomy should be reserved for highly selected patients and performed by surgeons with appropriate expertise [20].
Cortical tumors are particularly rare among children with AIs and are sometimes not clearly distinguishable from neurogenic tumors on preoperative imaging; in such patients, the presence of subclinical Cushing’s syndrome needs to be carefully evaluated preoperatively; otherwise, a perioperative adrenal crisis may occur [21]. In patients in whom the possibility of an adrenocortical tumor was considered preoperatively, the assessment for subclinical Cushing’s syndrome mainly involved assessing the serum dehydroepiandrosterone sulfate level and performing an overnight dexamethasone suppression test.
A procedure for evaluating pediatric AI is shown in Fig. 1. Imaging is the first step in the evaluation of AI in children. CT can be used to clarify the nature of most tumors. MRI can be used to evaluate imaging risk factors (IDRFs) for NB. Bone marrow cytomorphology is recommended for all children with AI, along with microscopic residual neuroblastoma testing and further bone scanning if the bone marrow examination is positive. In addition, serum tumor marker levels and other relevant tests should be performed, and hormone levels should be evaluated. If adrenal adenomas cannot be completely excluded during the preoperative examination, a 1 mg overnight dexamethasone suppression test should be performed to exclude subclinical Cushing’s syndrome. In patients with hypertensive hypokalemia, the presence of aldosteronism should be evaluated by testing plasma aldosterone concentrations and plasma renin activity. Adrenal masses found in the neonatal period can be observed if the tumor is small, confined to the adrenal gland and shows no evidence of distant metastasis, while tumors that increase significantly in size during the follow-up period or that are associated with persistently elevated tumor markers require aggressive surgical treatment.
Algorithm for the evaluation and management of a pediatric adrenal incidentaloma. *DST overnight :20µg/kg dexamethasoneweight ˂40 kg,1 mg dexamethasone if ≥ 40 kg. CT = computed tomographic;MRI = magnetic resonance imaging;NSE = neuron-specific enolase;AFP = alpha-fetoprotein;CEA = carcinoembryonic antigen;CA19-9 = cancerantigen19-9;ACTH = adrenocorticotropic hormone;PAC = plasma aldosterone concentration; PRA = plasma renin activity;DST = dexamethasone suppression test
The datasets analyzed during the current study are not public, but are available from the corresponding author on reasonable request.
Barzon L, Sonino N, Fallo F, Palu G, Boscaro M. Prevalence and natural history of adrenal incidentalomas. Eur J Endocrinol. 2003;149(4):273–85.
Maas M, Nassiri N, Bhanvadia S, Carmichael JD, Duddalwar V, Daneshmand S. Discrepancies in the recommendedmanagement of adrenalincidentalomas by variousguidelines. J Urol. 2021;205(1):52–9.
Fassnacht M, Tsagarakis S, Terzolo M, et al. European Society of Endocrinology clinical practice guidelines on the management of adrenal incidentalomas, in collaboration with the European network for the study of adrenal tumors. Eur J Endocrinol. 2023;189(1):G1–42.
Young WFJr. Clinical practice. The incidentally discovered adrenal mass. N Engl J Med. 2007;356(6):601–10.
Rowe NE, Kumar R, Schieda N, et al. Diagnosis, management, and follow-up of the incidentallydiscoveredadrenalmass: CUAguidelineendorsed by the AUA. J Urol. 2023;210(4):590–9.
Masiakos PT, Gerstle JT, Cheang T, Viero S, Kim PC, Wales P. Is surgery necessary for incidentally discovered adrenal masses in children?J. Pediatr Surg. 2004;39(5):754–8.
Lee JM, Kim MK, Ko SH et al. Clinical guidelines for the management of adrenal incidentaloma. Endocrinol Metab. 2017;32(2).
Terzolo M, Stigliano A, Chiodini I, et al. AME position statement on adrenal incidentaloma. Eur J Endocrinol. 2011;164(6):851–70.
Boland GW, Blake MA, Hahn PF, Mayo-Smith WW. Incidental adrenal lesions: principles, techniques, and algorithms for imaging characterization. Radiology. 2008;249(3):756–75.
Payabyab EC, Balasubramaniam S, Edgerly M, et al. Adrenocortical cancer: a molecularlycomplexdiseasewheresurgerymatters. Clin Cancer Res. 2016;22(20):4989–5000.
Angeli A, Osella G, Alì A, Terzolo M. Adrenal incidentaloma: an overview of clinical and epidemiological data from the National Italian Study Group. Horm Res. 1997;47(4–6):279–83.
Grumbach MM, Biller BM, Braunstein GD, et al. Management of the clinically inapparent adrenal mass (incidentaloma). Ann Intern Med. 2003;138(5):424–9.
Zhang K, Zhang Y, Zhang Y, Chao M. A retrospective analysis of the clinical characteristics of 207 hospitalized children with adrenal masses. Front Pediatr. 2023;11:1215095.
Nuchtern JG, London WB, Barnewolt CE, et al. A prospective study of expectant observation as primary therapy for neuroblastoma in young infants: a Children‘s oncology group study. Ann Surg. 2012;256(4):573–80.
Virgone C, Roganovic J, Vorwerk P, et al. Adrenocortical tumours in children and adolescents: the EXPeRT/PARTNER diagnostic and therapeutic recommendations. Pediatr Blood Cancer. 2021;68(suppl 4):e29025.
Chang S, Lin Y, Yang S, et al. Safety and feasibility of laparoscopic resection of abdominal neuroblastoma without image-defined risk factors: a single-center experience. World J Surg Oncol. 2023;21(1):113.
Zenitani M, Yoshida M, Matsumoto S, et al. Feasibility and safety of laparoscopic tumor resection in children with abdominal neuroblastomas. Pediatr Surg Int. 2023;39(1):91.
International Pediatric Endosurgery Group. IPEG guidelines for the surgical treatment of adrenal masses in children. J Laparoendosc Adv Surg Tech A. 2010;20(2):vii–ix.
Nakanishi H, Miangul S, Wang R, et al. Open versuslaparoscopicsurgery in the management of adrenocorticalcarcinoma: a systematicreview and meta-analysis. Ann Surg Oncol. 2023;30(2):994–1005.
Gaillard M, Razafinimanana M, Challine A, et al. Laparoscopic or openadrenalectomy for stage I-IIadrenocorticalcarcinoma: a retrospectivestudy. J Clin Med. 2023;12(11):3698.
Utsumi T, Iijima S, Sugizaki Y, et al. Laparoscopic adrenalectomy for adrenal tumors with endocrine activity: perioperative management pathways for reduced complications and improved outcomes. Int J Urol. 2023;30(10):818–26.
We would like to express our deepest gratitude to all the patients and their parents who participated in this study. Their patience and cooperation were instrumental to the success of this research. We thank our colleagues in the Department of Radiology for their invaluable contributions in diagnosing and monitoring the progression of adrenal incidentalomas. We sincerely appreciate the hard work of the pathologists in diagnosing and classifying tumors, which laid the foundation for our study. Finally, we would like to thank our institution for providing the necessary resources and an enabling environment to conduct this research.
Not applicable.
The authors declare no competing interests.
Ethics approval for this study was granted by the Ethics Committee of Children’s Hospital of Nanjing Medical University. Informed written consent was obtained from all the guardians of the children and we co-signed the informed consent form with their parents before the study. We confirmed that all methods were performed in accordance with relevant guidelines and regulations.
There are no conflicts of interest.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Filed under: Cushing's | Tagged: adrenal, adrenal carcinoma, dexamethasone suppression test, ganglioneuroma, neuroblastoma, pediatric, pheochromocytoma, subclinical Cushing's syndrome | Leave a comment »