Some diseases and conditions could be responsible for your abdominal fat.
Mita Majumdar | Updated: April 24, 2017 6:15 pm
Visceral fat or unhealthy belly fat that surrounds the liver and other organs in the abdomen puts you at risk for serious health problems, such as, metabolic syndrome, heart disease, and type 2 diabetes. But, what causes your pot belly or beer fat in the first place? The most obvious answers you will get is – ‘You are not exercising enough’, or, ‘you are eating too much of fatty foods or sugary foods’, or ‘you are not eating the right foods’, or ultimately, ‘It’s genetics! You got it from your parents’. All of these reasons are true, of course. However, some diseases/ disorders and conditions, too, could be responsible for your abdominal fat and these have nothing to do with not exercising or not eating right. Following are some of these disorders.
Cushing’s Syndrome
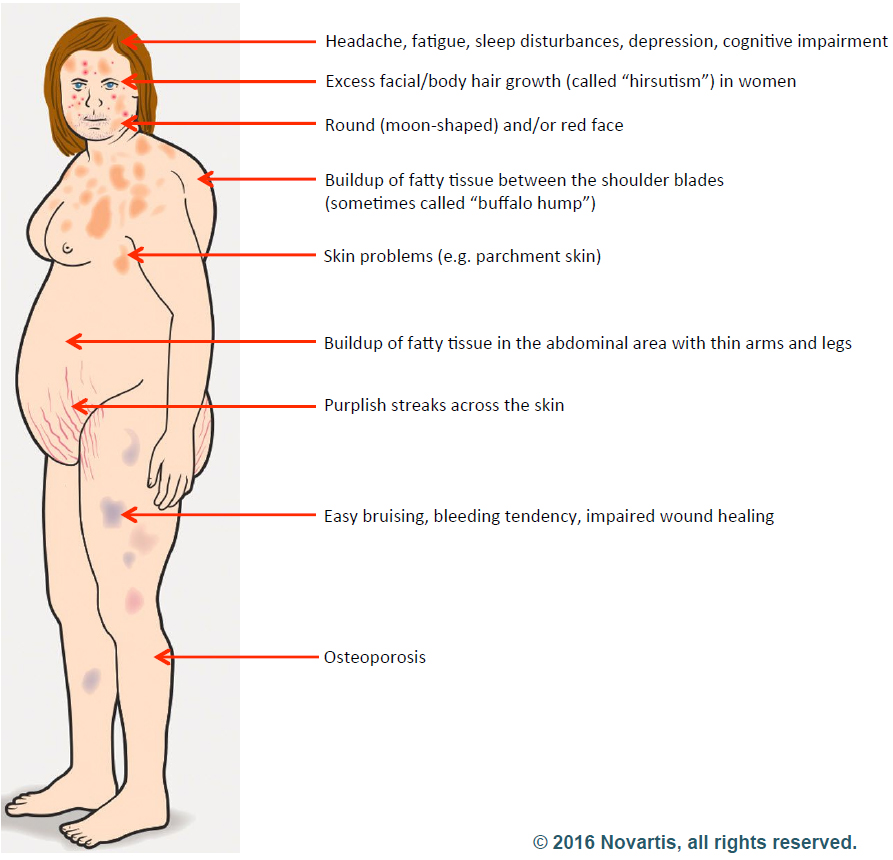
Cushing’s syndrome, also called hypercortisolism, is an endocrine disorder that occurs when your body is exposed to high cortisol levels over a long period of time. It is a treatable disorder, however, if it is chronic, the symptoms can last lifelong.
Symptoms: Symptoms vary according to the severity of the disorder. The characteristic symptoms include –
- Fatty tissue deposits in the midsection
- Fatty deposits in the upper back, especially between the shoulders, so that it resembles a hump
- Puffy face
- Violaceous stretch marks (pink or purple) on the arms, breast, stomach, and thighs that are more than 1 cm wide. [1]
- Easy bruising
- Fatigue
- Hirsutism and irregularity in menstruation in women
- Loss of libido and erectile dysfunction in men
- Cognitive dysfunction, depression, unpredictable emotional outbursts, irritability is present in 70-85 percent of people with Cushing’s syndrome.[1]
Causes:
- Overuse of corticosteroids
- Overproduction of cortisol by the adrenal glands
Management:
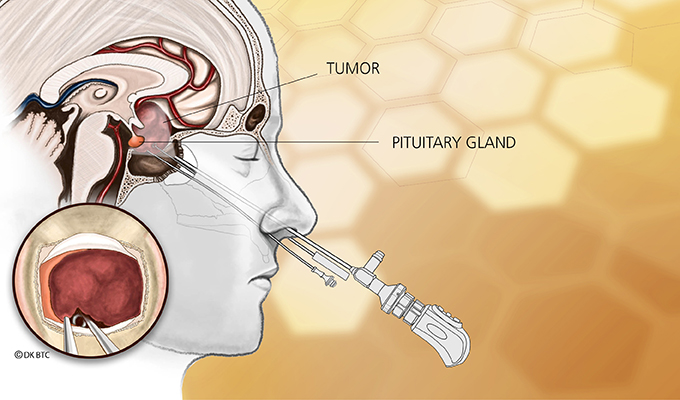
- Surgery is the first line of treatment for Cushing’s syndrome.
- Medication include: [2]
a.Pituitary gland directed therapy
b.Adrenal-blocking drugs
c.Glucocorticoid receptor-antagonizing drugs
- Pituitary radiotherapy
Addison’s disease
Addison’s disease, also called adrenal insufficiency, is a disorder where your adrenal glands produce insufficient hormones, especially, glucocorticoids including cortisol and aldosterone. It is a life-threatening disease that can affect anyone irrespective of their gender or age.
How do glucocorticoids influence abdominal fats? Glucocorticoids including cortisol convert the fats into energy in the liver. They also help your body respond to stress. When sufficient amount of glucocorticoids are not produced by the adrenal glands, the fats accumulate in the abdominal area, and you see it as flab around your middle.
Symptoms:
- Hyperpigmentation
- Extreme fatigue
- Low blood sugar and low blood pressure
- Salt craving as one of the functions of adrenal glands is to maintain the sodium-potassium balance in the body
- Nausea, vomiting, abdominal pain
- Weight loss but gain in abdominal fat
Causes:
- Insufficient production of adrenal cortex hormones
- Stopping of prescribed corticosteroids
- Tuberculosis and other infections of adrenal glands
- Spread of cancer to the adrenal glands
Management:
- Oral corticosteroids or corticosteroid injections
- Intravenous injections of hydrocortisone, saline solution, and dextrose in case of Addisonian crisis
Stress
Chronic stress is a very big cause of belly fat. When you are exposed to stress, a chain reaction starts in the body because of the dysregulation of HPA axis of the neuroendocrine system. HPA axis is a complex interaction between the hypothalamus, pituitary gland, and adrenal glands. The hypothalamus produces a corticotropin releasing hormone (CRH) and vasopressin. These together stimulate the secretion of adrenocorticotropic hormone (ACTH). ACTH is transported by the blood to the adrenal glands, which then produces corticosteroids, mainly, cortisol from cholesterol. One of the functions of cortisol is to signal the body to store fat, and specifically, the fat storage occurs in the abdominal area, where the cortisol receptors are greater. Researchers have found that stress causes hyperactivation of HPA axis, leading to accumulation of fat tissue, especially in the abdomen region.
So, the more and longer you are stressed (or if you are chronically stressed), chances are that you will be carrying more belly fat!
Ascites
Ascites is the buildup of fluid in the abdominal space. Ascites usually occurs in people with cancer, and it is then called malignant ascites. Onset of ascites is generally the terminal phase in cancer. Ascites also occurs in patients with liver cirrhosis, kidney failure, or heart disease.
Symptoms:
The first sign of ascites is an increase in abdominal girth accompanied by weight gain. [4] Although it looks like it is belly fat, it is actually the fluid that causes the bulging.
Other symptoms include:
- Shortness of breath
- Nausea and vomiting
- Swelling in the feet and ankle
- Decreased appetite, sense of fullness, bloating
- Fatigue
- Haemorrhoids
Management:
If the ascites is not causing any discomfort, it may not require any treatment. Treatment of ascites can have many side effects. Talk to your doctor before you go in for management/ treatment.
Abdominal hernia
Abdominal hernia is a swelling or a bulge in the abdominal area where an organ or fatty tissue pushes through a weak spot in the abdominal wall. The abdominal wall is made up of tough connective tissue and tendons that stretch from the ribs to the groin. Depending on the position of the weakness in your abdominal wall, the hernia can be inguinal (groin), femoral (upper thigh), umbilical (belly button), hiatal (upper stomach), or even incisional. Incisional hernia can occur when the intestine pushes through a weak spot at the site of abdominal surgery.
Symptoms:
- Visible bulge that may or may not cause discomfort
- Feeling of heaviness in the abdomen
- Sharp pain when you strain or lift objects
Causes:
- Constipation and diarrhoea
- Persistent coughing and sneezing
- Straining or suddenly lifting a heavy object
Management:
- Umbilical hernia, common in young children, mostly resolves by itself as the abdominal muscles get stronger.
- Other abdominal hernia normally do not resolve by themselves. Doctors suggest waiting and watching.
- If treatment is required, surgery is the only option. Surgery involves pushing the hernia back into the abdomen and repairing the abdominal wall.
Menopause
Menopause is certainly not a disease or a disorder. It is the time in a woman’s life when she stops menstruating and cannot become pregnant because her ovaries stop producing the required amounts of hormones oestrogen and progesterone. A woman reaches menopause when she has not had her periods for 12 months.
Symptoms:
- Hot flashes and/ or night sweats
- Vaginal dryness
- Mood swings
- Sleep disturbances
It is very common to gain belly fat during menopause. This is because of the low oestrogen levels. Oestrogen seems to influence the distribution of fat in the body, in a way that the fat is redistributed from the hips, buttocks, and thighs to the belly. However, a study published in the journal Metabolism reported that though women did significantly gain belly fat, especially deep inside the belly, relative fat distribution is not significantly different after menopause. [5] But the fact remains that women do gain flab in the abdomen after menopause.
Belly fat can be seriously harmful. If your belly fat is not because of the above-mentioned conditions, you can lose it by adopting a healthy lifestyle that includes sleeping enough, exercising regularly, eating right, and reducing stress.
Reference
- Sharma ST, Nieman LK, Feelders RA. Cushing’s syndrome: epidemiology and developments in disease management. Clinical Epidemiology. 2015;7:281-293. doi:10.2147/CLEP.S44336.
- Feelders RA, Hofland LJ. Medical treatment of Cushing’s disease. J Clin Endocrinol Metab. 2013;98:425–438.
- Kyrou I, Chrousos GP, Tsigos C. Stress, visceral obesity, and metabolic complications. Ann N Y Acad Sci. 2006 Nov;1083:77-110.
- Sinicrope FA. Ascites. In: Kufe DW, Pollock RE, Weichselbaum RR, et al., editors. Holland-Frei Cancer Medicine. 6th edition. Hamilton (ON): BC Decker; 2003.
- Franklin RM, Ploutz-Snyder L, Kanaley JA. Longitudinal changes in abdominal fat distribution with menopause. Metabolism. 2009 Mar;58(3):311-5. doi: 10.1016/j.metabol.2008.09.030.
Adapted from http://www.thehealthsite.com/diseases-conditions/reasons-you-have-flab-around-your-abdomen-f0417/
Filed under: adrenal, Cushing's, Rare Diseases, symptoms | Tagged: Addison's disease, adrenal insufficiency, Ascites, cortisol, Cushing Syndrome, Dr. Lynnette Nieman, fat, hernia, hypercortisolism, menopause, weight | Leave a comment »