Your hair can tell you and your doctor if you are stressed, have a nutritional deficiency, thyroid problem, or other health issues. Here are seven key things to look for in your hair.
You probably think about your hair every day: worrying about a bad day, enjoying a good blow-dry, or wondering if you have to try the new style you noticed in your favorite celebrity. But you may be missing the clues your hair reveals about your health. Research shows that changes in the look, texture, or thickness of your hair can be signs of underlying health issues. Here’s how to tell if your hair changes are due to a health condition, genetics, stress, or a nutritional deficiency.
1 Stress (and genes) can cause you to turn gray
Anyone who has observed the hairstyle changes of a President of the Republic from one campaign to another has noticed that stress seems to cause hair to turn white. A mouse study published in the journal Nature suggests that chronic stress may actually contribute to white hair by causing DNA damage and reducing the number of pigment-producing cells in hair follicles. Stress can also lead to hair loss.
Another type of stress, known as oxidative stress, can also play a role in white hair. Oxidative stress can affect pigment-producing cells. Turning gray is actually a completely natural part of aging because hair follicles produce less color as you age. Your genes also play a role in when your hair turns gray. Ask your parents how old they were when they first saw the signs of silvering, and you might do the same. In fact, a study published in March 2016 in the journal Nature Communications was the first to identify the gene responsible for white hair.
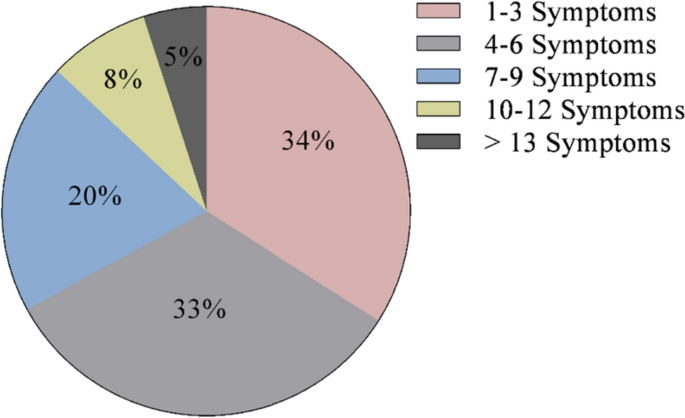
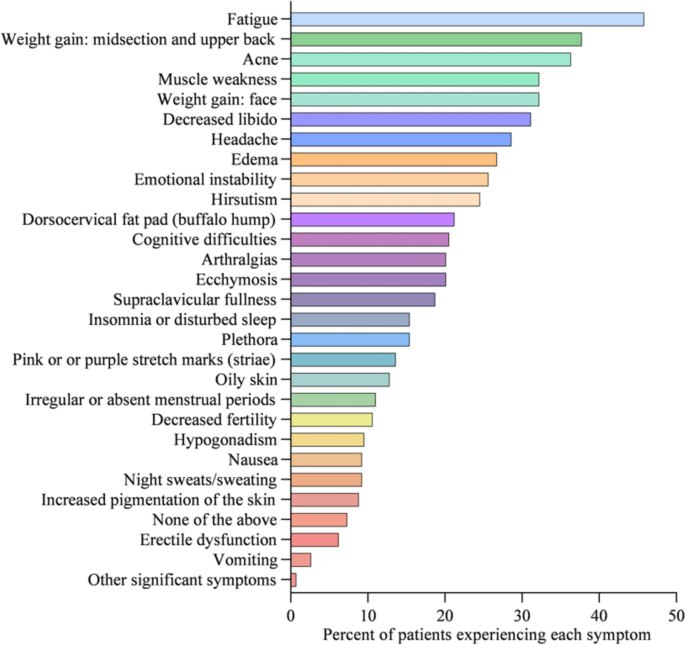
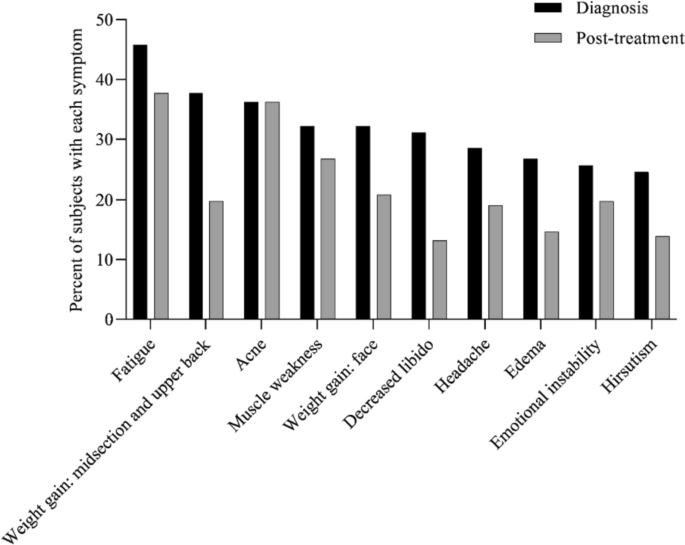
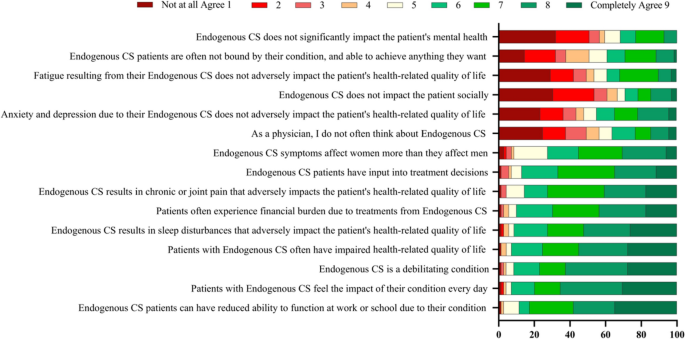
2 brittle hair could be a sign of Cushing’s syndrome
Brittle hair is one of the symptoms of Cushing’s syndrome, which is a rare condition caused by excess cortisol, the main hormone body stress. But, there are many other, more obvious symptoms of Cushing’s syndrome, including high blood pressure, fatigue, and back pain. Treatment for Cushing’s syndrome may involve changing the dose of medication that may be causing the condition, such as glucocorticoids, which are steroids used to treat inflammation caused by various diseases.
3 Thinning hair may be a sign of thyroid disease
People with hypothyroidism, a condition that occurs when the thyroid gland does not produce enough thyroid hormones, may notice increased hair loss and change in hair appearance. About 4.6% of the population aged 12 years and older have hypothyroidism, although most cases are mild. Hypothyroidism can lead to thinning hair and other symptoms, such as fatigue, intolerance to cold, joint pain, muscle aches, puffy face and weight gain. A thyroid stimulating hormone (TSH) test can diagnose the condition, and treatment involves taking thyroid medication.
In addition to thinning hair, some thyroid disorders put you at risk for risk of autoimmune hair loss called alopecia areata. This type of hair loss causes round patches of sudden hair loss and is caused by the immune system attacking the hair follicles.
4 Hair loss can be a sign of anemia
If you suddenly notice a lot more hair in your hairbrush or on the floor of your shower, it may be a sign that your body has low iron stores, or anemia , and may warrant testing. This is another blood test we do when you complain of hair changes. Vegetarians or women with heavy periods increase their risk that hair changes are due to iron deficiency.
It is unclear why iron deficiency can lead to hair loss. hair, but iron is essential for many biological and chemical reactions, perhaps including hair growth. Hair loss can also occur (temporarily) with sudden changes in estrogen levels and is often noticed after pregnancy or stopping birth control pills.
5 The loss of hair could indicate protein deficiency
Protein is essential for hair health and growth (a lack of protein has been linked to hair thinning and hair loss ). Protein deficiency is not a problem for most people. Most adults need 0.8 grams of protein per kilogram of body weight. Good sources of protein include low-fat Greek yogurt, chickpeas, and chicken breast. People who have gastrointestinal difficulties or who have just had gastric bypass surgery may have problems digesting protein. These special situations will need to be managed with the help of your doctor. But most cases of thinning hair, even in women, are probably due to genetics.
6 White or yellow flakes can mean you have dandruff
Yellow or white flakes in your hair, on your shoulders and even in your eyebrows are a sign of dandruff, a chronic scalp condition. Dandruff is usually not a sign of a health problem and can be treated with specialized over-the-counter or prescription shampoos.
One of the most common causes of dandruff is a medical condition called seborrheic dermatitis. People with seborrheic dermatitis have red, oily skin covered in white or yellow scales. A yeast-like fungus called malassezia can also irritate the scalp. Insufficient shampoo, sensitivity to hair care products, and dry skin can also cause dandruff. (Dandruff is usually more severe in the winter, when indoor heating can make skin drier).
7 Damaged hair can mask other health issues
Although hair can reveal your condition, women more often complain about the damage caused by hair coloring and heat treatment. Excessive heat, from daily use of a flat iron or blow-drying, can certainly damage your hair, making it dry, brittle and difficult to maintain. Best not to use more than one hot tool per day (occasional double heat treatment is okay, but not daily). When applying heat to your hair, always use products with protective ingredients. Serums and shine drops tend to have hair-preserving qualities when using direct and indirect heat.
From https://www.mvdemocrat.com/appearance-texture-thickness-7-things-your-hair-reveals-about-your-health/
Filed under: Cushing's, symptoms | Tagged: back pain, cortisol, fatigue, high blood pressure, stress, thyroid | Leave a comment »